I was taking care of my best friend in hospice, and then we both got COVID-19.
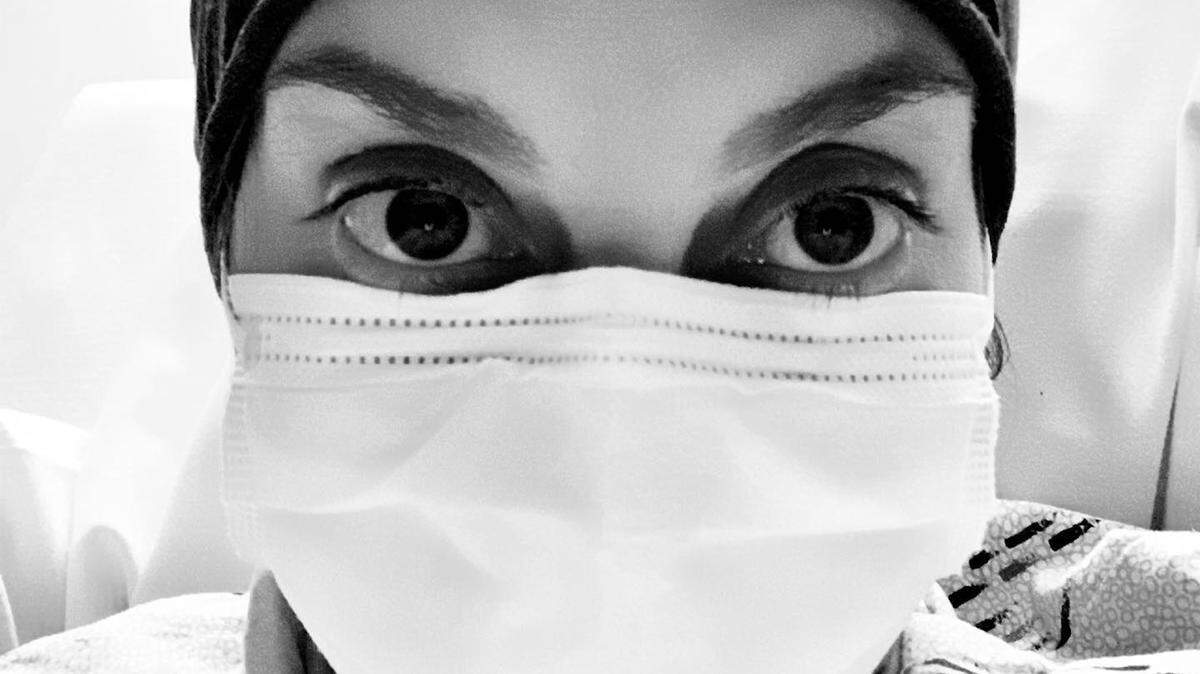
Editor’s note: Winthrop University alumna Mel Umbarger, who now lives in Greensboro, drove to Florida during COVID-19 to take care of her best friend as she was dying of a genetic disease. She had been quarantined since March, so she felt safe. Then one night, a home health aide showed up with a cough.
My best friend didn’t die of COVID-19. But COVID-19 would make a huge difference in the way she died.
Colleen Davis would have turned 40 on Sept. 28, but she died more than a month short of that. At 3:23 p.m. on Aug. 19, she passed away at home as I was holding her hand. Despite her many family members and friends, the only other ones there were the hospice doctor and her three cats.
Despite all our precautions since mid-March, we had both been exposed to COVID-19 while quarantining together at her home while she was in hospice care. I tested positive, she tested negative, but we both got the symptoms.
A lifelong friendship
We met nearly 30 years ago when we were in the sixth grade in Daytona Beach, Fla. We bonded over our love of books and grammar, our shared worry that people would stare at the teeth marks in our sandwiches and Guns N’ Roses.
I don’t remember everything we talked about on the phone after school, but we stayed connected for hours at a time. And we’d go on to stay connected for the next 29 years — through the years I spent at Winthrop University in Rock Hill and she spent at California State University, Fullerton; then getting married, and then moving on with life in states far apart. I ended up in North Carolina, she in New England.
Neither of us had blood sisters, but we had found a sister in each other.
When she was 27, she told me that she had been diagnosed with Ehlers-Danlos Syndrome, she was getting divorced and she was moving back to Florida.
EDS is a genetic disease that affects connective tissue in the body — which pretty much everything in the body is made of, including skin, organs, veins and more. There are several types of it, and she had one of the more severe. I’ve heard the analogy of a house made of faulty materials — it still looks like a house, but because all the materials are poor, issues can pop up anywhere.
She lived on her savings for some time, while she waded through the bureaucracy of Medicaid and the Florida disability program. Her divorce meant that she lost access to health care insurance.
Being sick during COVID-19
On May 8, 2020, she ended up going into the hospital in Daytona for ongoing stomach problems, and she was in serious pain. Other symptoms led her to worry she had COVID-19, but a test revealed she had the flu instead.
According to the Florida Department of Health, on May 8, there were 39,199 cases and 1,669 deaths due to COVID-19 in Florida. The headline that day was that Florida Gov. Ron DeSantis announced that barbershops and salons could reopen.
The hospital was clearly struggling to maintain COVID-19 guidelines. It took some time for them to even find her a bed. She posted this on May 12 on Facebook:
“I’ve been exposed to healthcare workers coughing and wiping their faces because they can’t breathe through a mask and don’t have gloves on, and they took my test sample Thursday and put it into the rapid return system since you have to know if someone inpatient has it or not ASAP, but it’s now Tuesday and I don’t have results back because this is a political nightmare ...”
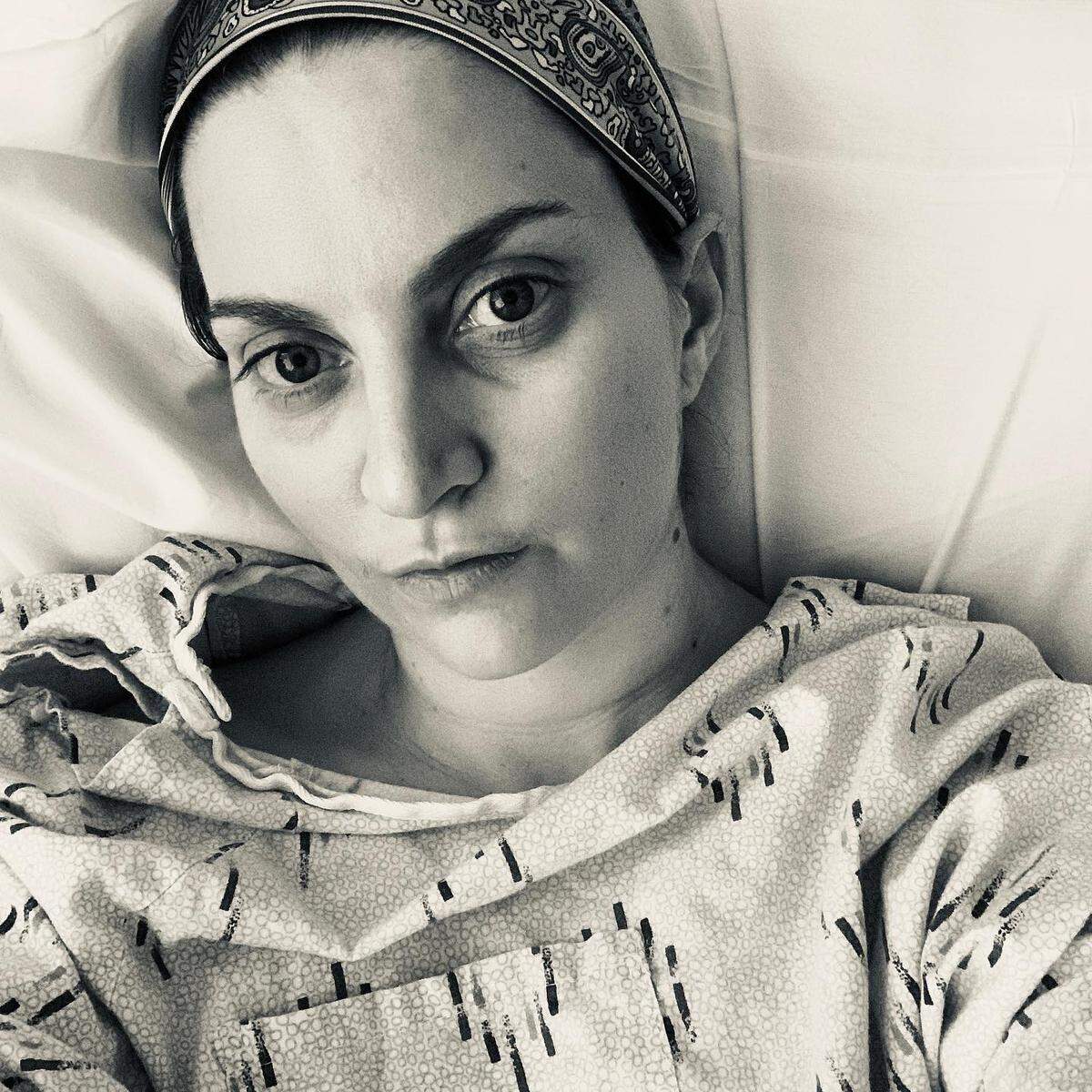
By June 1, when she was moved to an Orlando hospital with better facilities, she was in bad shape. The feeding tube they tried twice to put in wasn’t working and she was in more pain.
On June 1, the headline in the Orlando Sentinel read, ”Florida adds 667 coronavirus cases for total of 56,830; death toll at 2,460.”
She ended up in a room the size of a closet with a faulty hospital bed and no A/C. There was nowhere else for her to go because of how COVID-19 was affecting everything. I asked if I could drive from Greensboro to visit her, and she told me that they were only allowing one family member a day to visit because of the pandemic.
Sisters of the heart didn’t count.
Over the next month, it was a roller coaster of symptoms and complications, and the maelstrom of a pandemic in a major hospital meant that her nurses were overworked and things fell through the cracks. They decided to discharge her with a plan for home health care on July 1.
The promised support didn’t materialize, and she was miserable and in pain. I texted her when it became clear she wasn’t going back to the hospital immediately. “Are you staying at home? If so, I will come down and stay with you. I can bring an air mattress and sleep wherever.” She called me back and said yes.
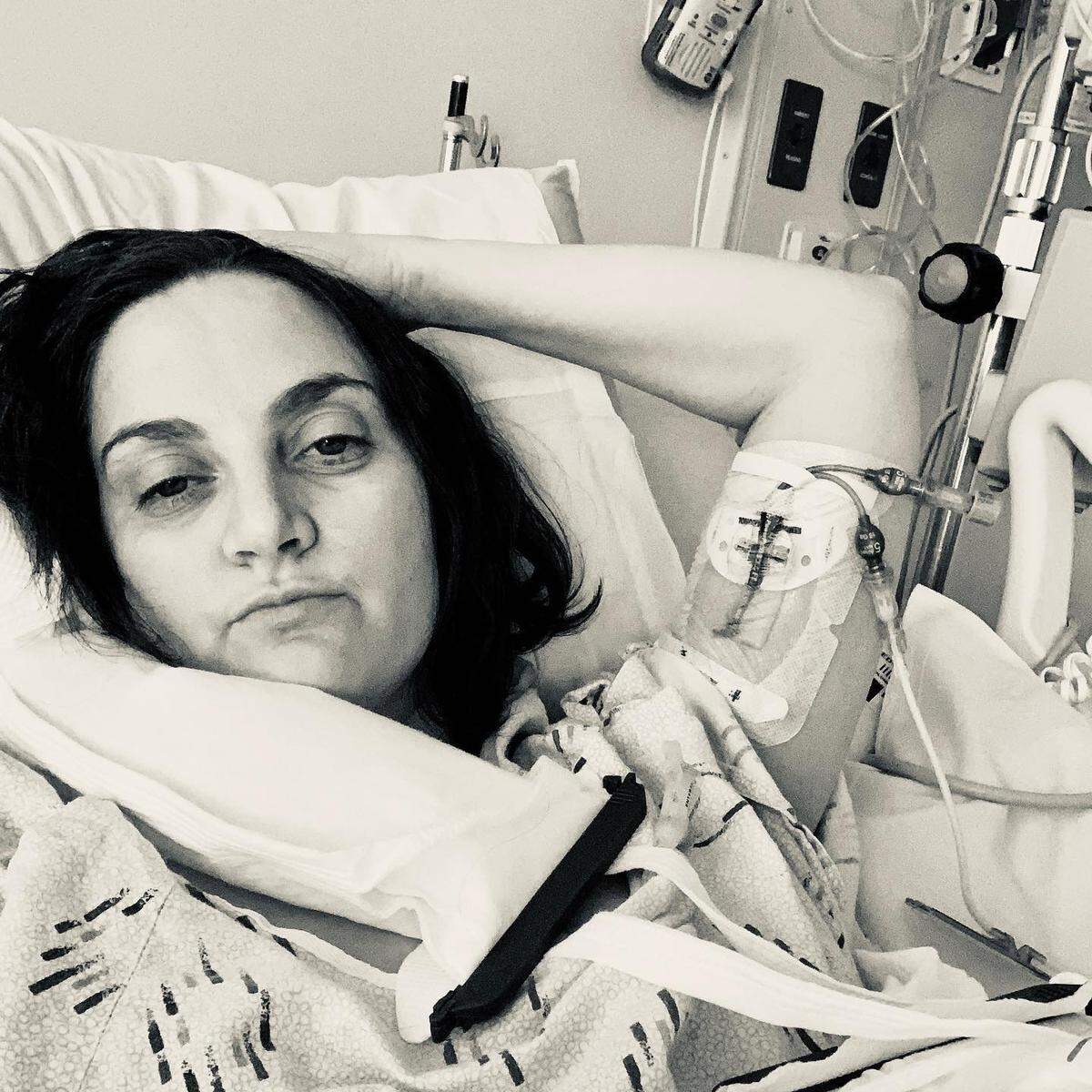
I had been quarantining since March with my husband, so I knew I was safe. I had been working from home, so I could continue to do my job from Florida. She started talking about hospice at this point to me and some other friends, but was worried everyone would fault her for giving up.
“I love you,” I told her. “I’ll never fault you for any decision you make.”
The machines keeping her alive at home started to fail, and she wasn’t staying hydrated enough. By July 7, she returned to the hospital in Orlando. She posted this:
“I will say, however, because I was assuming to not be able to speak or hear when I was brought here, I’m not sure why, my gurney was inadvertently placed in a staff only section where physicians were meeting and quite upset, because there are no intensive care beds left, and the emergency department has no ability anymore to really place people on holding, and have no idea what to do with people who need intensive care, or I think really even critical care at this point, because the hospitals just at capacity.”
On July 7, the Florida Dept of Health announced a total of 213,794 Florida cases, with 3,841 deaths related to COVID-19.
On July 12, her doctors were still pushing an experimental procedure on her that would only have a possibility of relieving one of her symptoms. She told them she wasn’t interested and wanted to talk about hospice.
Hospital visiting during COVID-19
She was still in the hospital when I headed down on July 17. Patients could have one visitor a day at this point because of the pandemic, so we had to text with her mom and dad to determine which days I could visit her.
Visiting her meant lining up each day at the hospital check-in area to get my temperature taken, answer the COVID-19 exposure questions and be issued a disposable mask to be worn constantly. I was really uncomfortable with the number of people I passed on the way into the hospital who weren’t covered up.
On July 22, she was able to go home under hospice care. We had constant support — 24-hour care for the first week from hospice, daily visits from her mom to relieve me for a couple hours a day, and overwhelming generosity from our friends and family.
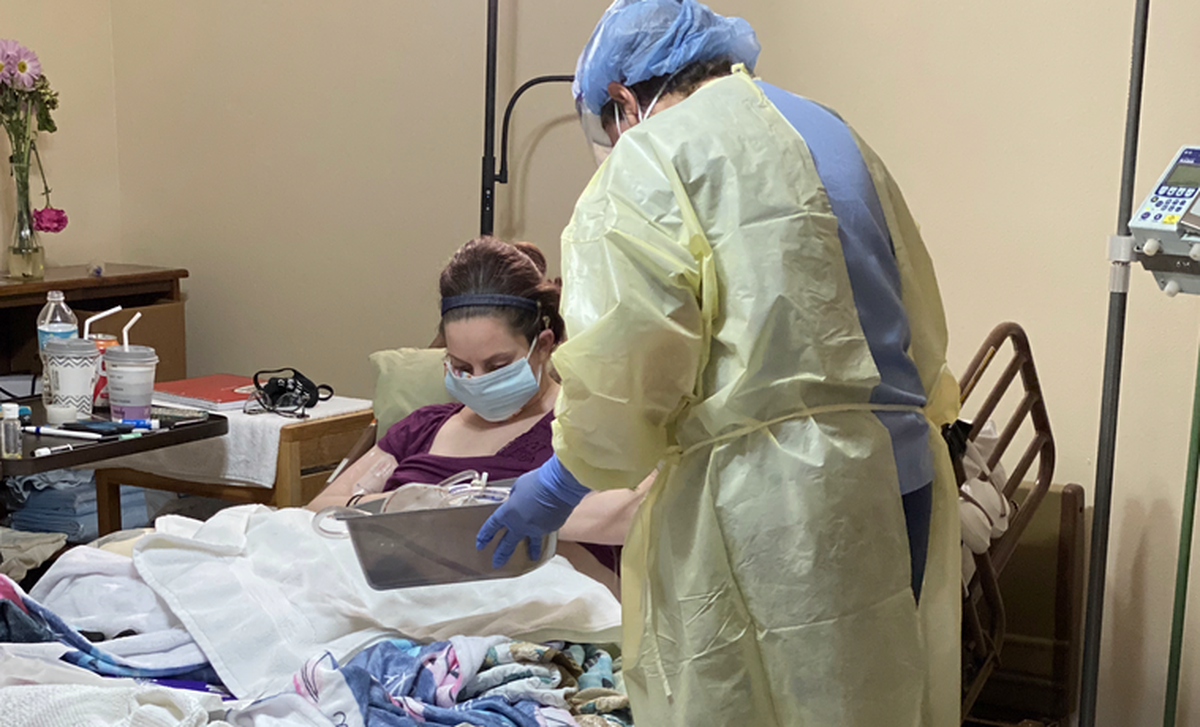
Several Amazon packages arrived daily with things to make her more comfortable. (“Seasons of Love” never talked about measuring your life in Amazon boxes,” she told me.)
My mom, who still lives in Florida, dropped off homemade comfort foods on the doorstep for dinner. Colleen’s dad had been traveling recently, and he was waiting out the two-week quarantine before he could see her in person. Everyone who came into the house wore a mask, and so did we.
Then hospice transitioned her from 24-hour care to a nurse checking in on her daily. Colleen’s mom made arrangements with a home health agency to send someone at night.
From best friend to caregiver
I’m not going to say that being Colleen’s primary hospice caregiver was fun, but we got to spend more time together than we had in years. We talked for hours, sitting up as long as she could, usually late at night after her pain meds kicked in a bit. We reminisced about our younger years, we laughed and watched bad reality TV together.
They had converted her feeding tube to just a drainage tube, so she could eat and drink for comfort. She took advantage of that, eating all the sweets she wanted. I stocked the fridge with salted caramel and bananas foster cashew milk ice cream, key lime pie and mango key lime pie from Publix, and toaster strudels. And sweet tea, of course.
We talked about her wishes, and I kept notes. We wrote her will. We arranged to donate her body to science. And we talked about her decision and her fears. And every time I walked out of the room, we said, “I love you.”
It was scary, and I often felt like I was in over my head. One night, there was a complication and a nurse offered to take Colleen back to the ER. She said, “I’d rather die than go back to Halifax hospital,” and we both started laughing through the tears. We laughed even harder when the nurse repeated her words in a deadpan tone to the doctor on the phone. Dark humor had always bonded us.

Colleen then had to make a pretty instant choice to stop either her pain pump or nutrition. It was easy for her. She chose to stop her nutrition, and they upped the pain medication to make the coming days easier.
The next call: A COVID-19 diagnosis
On Aug. 3, Florida had 491,884 total cases of COVID-19, 7,157 deaths, and 27,366 hospitalizations.
The previous Thursday night, a home health worker showed up with a cough to care for Colleen. I asked her if it was COVID-19, and she assured me it wasn’t. Still, at 1 a.m., her cough was keeping Colleen awake, so we asked her to leave. I saw her face when I asked her if she would be paid for the rest of her shift, and she told me no. I handed her some cash on the way out. I am angry, however, at a system that allows a healthcare worker to be paid $8 an hour without sick time.
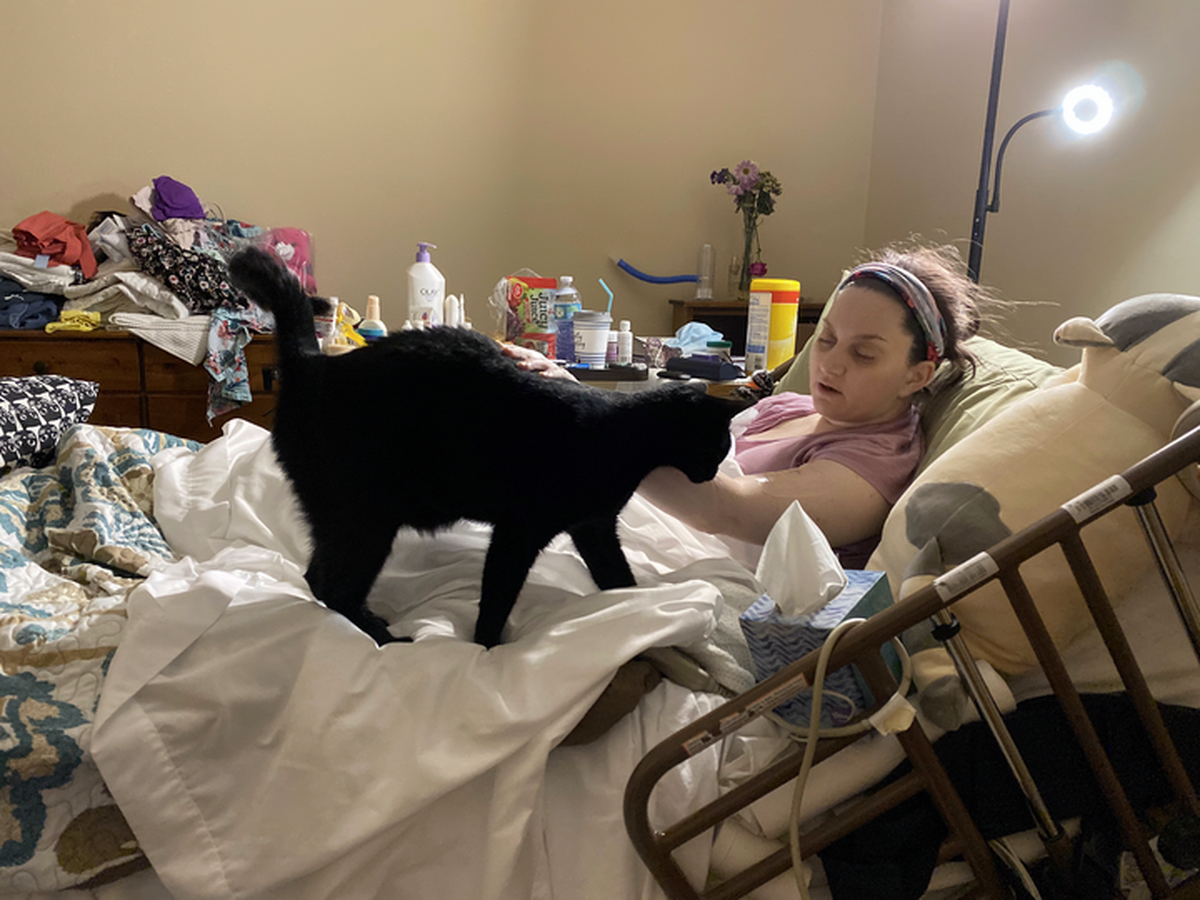
A few days later, we got a call from Colleen’s mom: The home health aide had tested positive for COVID-19.
Colleen’s parents couldn’t visit until we were both tested and cleared. If one of us tested positive, they’d have to wait two weeks to see her — and she likely didn’t have two weeks.
Colleen was tested on Aug. 4 and was negative. I was tested on Aug. 5 and was positive. I sat in the parking lot of the urgent care and sobbed to my husband on the phone. After I calmed down, I called Colleen. We cried together some, then talked. Her voice was tired when she said, “Just come home. It’s not like I can die twice. We’ll get through this together.”
Before I headed to her home, I talked to her dad. We arranged for her to sit in her wheelchair on her front step, and he stayed 6 feet away while they visited for a couple hours.
When hospice found out, all nursing switched to FaceTime visits. Unfortunately, the wonderful nurse who had come over that weekend to help Colleen had to be quarantined for 14 days, as did her hospice case manager nurse. It also meant that goodbye visits with some of her friends couldn’t happen.
‘I got sicker, so did she’
On Aug. 6, I started showing symptoms. It became exhausting just to walk from one room to another. Despite her negative COVID-19 test, Colleen started having some symptoms. Her nurse was convinced she had been tested too early.
Over the next few days, I developed a cough, and I ordered an oxygen monitor for my finger. I got night sweats, and I added achiness and headaches to the list. I also started forgetting things very easily, and I was unsure whether to attribute it to COVID-19 or exhaustion.
As I got sicker, so did she.
Hospice sent a nurse in complete PPE to install a new pain IV. As we talked with him, we found another North Carolina connection — he grew up in Welcome, N.C., and Colleen had spent her younger years in Durham.
She also developed a deep cough.
‘I started getting better, and she started to decline.’
As we struggled, our community stepped up to help. My mom continued to leave food on the doorstep. Our friends continued to send helpful things, notes of love and flowers. My co-workers raised more than $600 for gift cards for food. I burned through my paid time off and two weeks of COVID-19 leave, so my co-workers donated their leave as well. I have never been more thankful.
We spent the next few days sleeping to the sound of Florida thunderstorms.
I started getting better, and she started to decline.
On Aug. 13, I took my first shower in more than a week, which left me exhausted. And the doctor started her on a heavy sedation drug every two hours.
According to the Florida Dept of Health, as of Aug. 13, there were a total of 563,285 Florida cases with 9,141 deaths related to COVID-19.
Over the next couple of days, she stopped waking up. I whispered the love and support from her friends and family to her, and her sweet cat Chucks stayed curled on her bed constantly. Her other two cats came to visit, too. I ran her hands over their fur, hoping she would know they were there.

On Aug. 18, I tested negative for COVID-19, though my symptoms weren’t gone. The doctor came by to check on her, and he told me it would likely be less than 48 hours. Her mom sat with her and said goodbye while I ran an errand.
The next day, the doctor stopped in again. He thought it would be at least another 24 hours. We stood there in her room and talked a little bit more, and then he looked over at her. “It’s happening now.” She has always been precocious, and she would have been thrilled to stay on brand even in her death.
He left the room, and I texted her dad to hurry for his planned afternoon visit. Then I held her hand and said goodbye.
As of Aug. 19, Florida had 584,047 cases of COVID-19. It passed 10,000 deaths due to COVID-19, but Colleen was not one of them.
COVID-19 struggles, even after death
Even after her death, COVID-19 continued to affect her. I was unable to carry out her wishes in some cases because of how things have shut down. The domestic violence shelter she asked me to donate many of her things to was not taking physical donations due to the pandemic.
Her funeral service was supposed to be streamed online, but technical problems meant no one got to see it. Her friends and family have grieved apart.
I continue to recover from COVID-19. I am probably 90% back to normal. I can make it through most work days now, although I still had to tap out early for a nap one day last week. I am still struggling mightily to find words that are on the tip of my tongue, and the ones that come out are wrong more than I like. Not remembering names of people and places that I can see clearly in my mind.
As I write this, I just finished emptying Colleen’s bookcases. It’s one of the things I left ’til last because I knew it would be one of the hardest. Tucked into many of her books, I found notes and recipes in her handwriting, pressed flower petals, receipts and the detritus of life that we bookworms often turn into bookmarks.
It feels like she is disappearing, piece by piece, as I empty her house. But I know she won’t ever be completely gone — she has too many friends and family members who will remember the kind, brilliant and compassionate woman who so loved her cats and her family, both chosen and blood.
I just hope that her story can inspire others to wear their masks and take this seriously. Just one person with COVID-19 can affect so many lives in an ever-widening ripple effect.
How you can help
Contact your lawmakers and tell them to expand Medicaid. Or disability rights. Or anything that may keep your best friend alive in the future. NCjustice.org/take-action/
For more information about hospice in your area: http://www.nationalhospicelocator.com/
Many universities and research centers in North Carolina participate in donation programs. Organ donors cannot donate their bodies to science. https://coa.dph.ncdhhs.gov/donate.htm
This story was originally published October 7, 2020 at 12:30 PM.