Where exactly do people get COVID-19 in Charlotte? For the most part, no one seems to know.
Health officials have publicly linked less than 5% of the more than 21,000 known coronavirus cases in Charlotte and its surrounding towns to a specific location.
That leaves more questions than answers about where people most-recently diagnosed — nearly 9,300 in July alone — contracted the virus.
In some cases, restaurants and other businesses have opted to self-disclose when a handful of employees test positive. In other instances, local daycares, nursing homes and other living facilities are required to promptly tell local health departments about outbreaks.
Since late-March, local government leaders have been warning the risk of infection lurks any place where strangers, friends or family might gather, particularly in large groups indoors. That, in large part, has led to restrictions on restaurants and bars, delaying in-person learning for public schools and a wide-range of other pandemic-induced shutdowns.
But for the vast majority of COVID-19 cases in and around the Charlotte area, health officials don’t know the location of exposure or how many people may have come in direct contact with a contagious individual.
“We’ve got widespread community involvement. Widespread. Trying to figure out where individuals actually picked this up is very hard to do,” Mecklenburg Public Health Director Gibbie Harris told the Charlotte Journalism Collaborative, which includes the Observer.
There’s a similar conundrum across North Carolina: Only about 1 in 10 cases have been traced back to “congregate living” settings, which includes jails, nursing homes and senior living facilities. Details on other specific hotspots are virtually unknown to the public.
Public health directors statewide are relying on an unwieldy strategy — known as contact tracing — intended to pinpoint coronavirus clusters and prevent infectious flare-ups.
The Observer talked with infectious disease experts and health department officials in counties across the Charlotte region. Many share concerns about the effectiveness of contact tracing, particularly as hundreds of new cases per day are added to investigators’ workloads.
“It begins to feel like putting out a wildfire with a spray bottle,” said Jim Thomas, a social epidemiologist at UNC Chapel Hill who studies pandemic ethics.
“It’s very daunting, if not depressing. That doesn’t mean they shouldn’t be doing it.”
Mecklenburg health authorities say large gatherings at places like churches or nightclubs can become COVID-19 hotspots. But officials struggle to effectively — and definitively — connect new outbreaks to specific houses of worship, bars and restaurants.
“The information that we get — the name of the restaurant and the date and time they went and all of that — it’s been challenging to try and place that all together,” Dr. Meg Sullivan, the county’s medical director, told the Observer. “That’s something we’re continuing to strive to do.”
The most pressing contact tracing challenges include:
▪ Mistrust or unwillingness to provide private health and contact information by phone. It’s particularly a concern among lower-income communities disproportionately impacted by the coronavirus.
▪ Lengthy turnaround times for COVID-19 test results
▪ Shortage of case investigators and contact tracers
▪ Widespread community transmission of the virus
‘Everyone doesn’t agree’
Public health experts warn that by the time a person receives a positive test result, they might have been unknowingly spreading the virus for days throughout the community. That creates a dizzying domino effect, in which a patient may not accurately remember who they’ve interacted with and likely has no reliable way to identify people they sat next to in a restaurant, for instance.
And then there’s the problem of people not picking up their phone when a health department contact tracer calls from a number they don’t recognize.
Once contact is made, some patients are wary of providing their employer information, believing they could be fired or punished. Others fear being ostracized by friends and family for getting them sick, health experts say anecdotally. Others refuse to self-isolate for a full two weeks.
“Everyone doesn’t agree on the things we recommend,” said Ellen Wright, a lead communicable disease nurse in Gaston County. “There’s only so much we can do. A lot of this responsibility is placed on the individual.”
Harris said Mecklenburg is weighing the merits of ongoing contact tracing efforts with the Centers for Disease Control and Prevention, as well with state health leaders. The county may slow down the program, Harris said, or “crack down on enforcement” as people fail to cooperate with contact tracers.
Still, when contact tracers do piece together the virus’ spread, the results are striking.
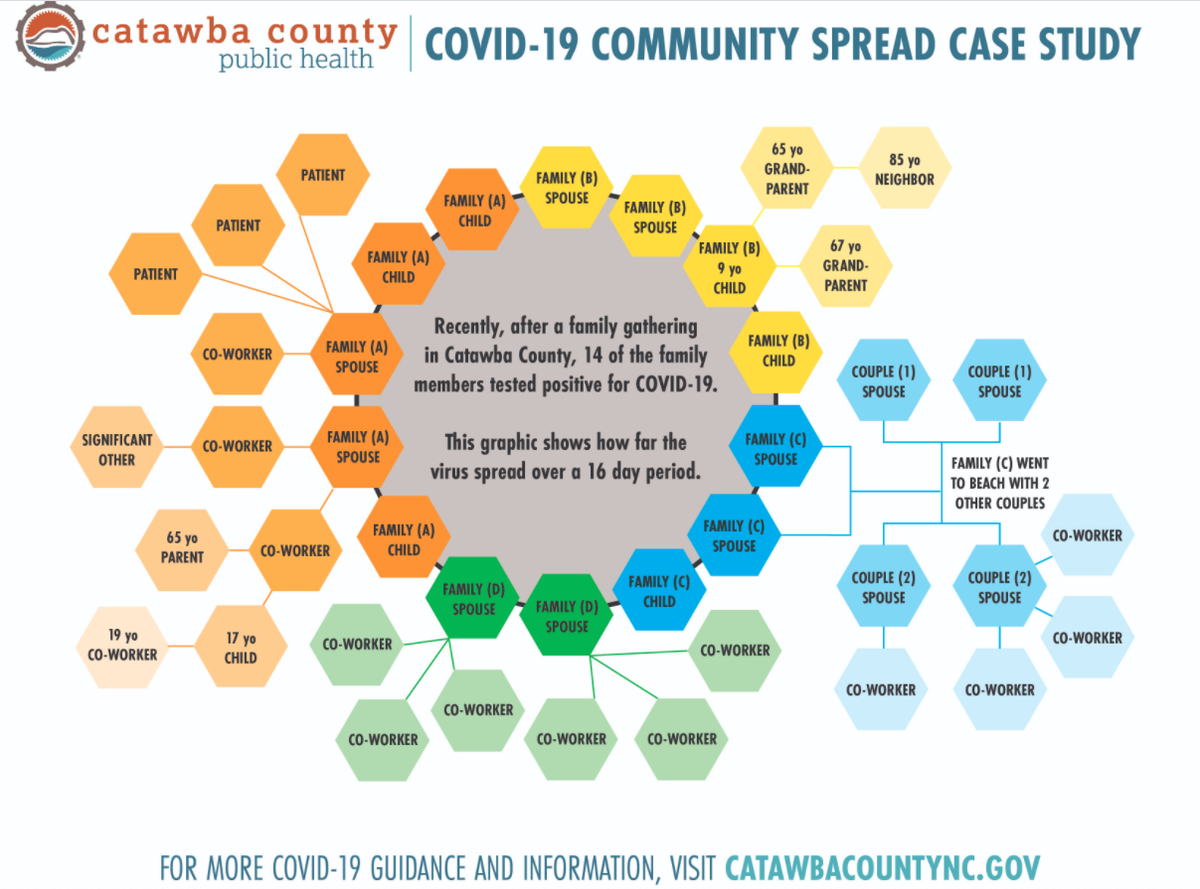
In Catawba County, the health department linked at least 41 coronavirus cases to a single family gathering where people did not wear masks or follow social distancing guidelines, the Observer previously reported.
But health officials told the Observer that successful case studies like this are rare, with contact tracers more often than not juggling fragmented bits of information.
What is contact tracing?
The COVID-19 case investigation process — the first step of a contact tracing program — is supposed to launch within 24 hours of a lab-confirmed diagnosis, according to July guidance from the state Department of Health and Human Services.
Investigators call infected individuals to gather basic information about their recent close contacts, defined as those who stood within 6 feet of them for at least 15 minutes.
“When you really break it down, the list narrows,” Wright said. “That makes it easier for us to get those contacts, especially within the workforce — rather than having to test a whole facility.”
Investigators are trained to probe for contacts’ names, employers, phone numbers and home addresses, among other details. Generally, the queries are straightforward and not difficult for people to answer, Wright said.
In a script for case investigators in North Carolina, officials recommend a caller appeal to a person’s sense of duty to keep others stay healthy: “In an effort to help prevent COVID-19 from spreading to others within your household and community, I need your help to identify individuals you have been in close contact with during the period of time you may have been contagious.”
Contact tracers then use that information to call people potentially exposed. They ask about symptoms such as a fever or difficulty breathing.
Crucially, contacts tracers urge people to get tested for the virus and to self-isolate. Such steps, public health experts say, are proven to help break the transmission chain.
But contact tracers in North Carolina lack surveillance or enforcement tools to confirm whether infected individuals stay home or venture out, possibly propagating COVID-19.
To avoid that scenario, both case investigators and contact tracers also ask what resources COVID-19 patients may need, such as groceries to last for the 14-day quarantine or a referral to a primary care physician. Based on state guidance, some questions include:
▪ “Are you able to stay home from work and not leave the house for up to 14 days?”
▪ “Do you have a stable and safe place you feel comfortable staying in for the duration of this stay at home period?
▪ “Do you have the ability to isolate yourself within your home away from others?”
▪ “Do you have any household (members) that are high risk for complications should they become infected?”
Throughout the isolation period, patients opt into automated text messages, emails or phone calls that remind them to follow health recommendations.
All of this, though, is dependent on whether health department workers are even able to reach a person diagnosed or possibly exposed. Then after clearing that obstacle there are other problems: delays in test results, a staffing crunch and the seemingly-insurmountable challenge of tracking the transmission of a novel airborne virus.
‘Formidable’ hurdles
The backlog in COVID-19 test results — which has recently spanned up to 10 days — stifles contact tracing efforts, officials say. Infected individuals and their close contacts may end up missing the critical time window to quarantine.
“Absolutely, the effectiveness is less the longer those turnaround times are,” Sullivan, Mecklenburg’s medical director, said. “The whole goal of case investigation and contact tracing is to first make sure the person who tested positive is isolated.”
The CDC has said a person is contagious beginning two days prior to showing symptoms and until 10 days after they first appear. Asymptomatic coronavirus patients can spread the virus without even knowing it or realizing they’re sick.
With a testing backlog of even just a few days, health officials are handcuffed from the start of contact tracing efforts.
Contract tracing went smoother in February, when health officials were only monitoring international travelers from China and the coronavirus had yet to be detected in North Carolina. At least under the most-restrictive stay-at-home orders this spring, people had limited interactions with people beyond their households, Sullivan said.
Previously, officials have seen when infections spread in a more limited network — such as with sexually transmitted diseases — contact tracing is much more effective, said Thomas, of UNC Chapel Hill.
Infected individuals can more easily recall their close contacts, and contact tracers, in turn, contend with fewer people to call.
By contrast, tracing a highly-contagious respiratory illness poses “formidable” hurdles, Thomas said, particularly at this juncture of the pandemic when hundreds of new cases are detected daily in Charlotte.
Health departments are further strained by limited staff resources.
In Mecklenburg, the health department has turned about 50 school nurses into coronavirus case investigators. With only remote learning planned for now at Charlotte-Mecklenburg Schools, some of those nurses “will be able to continue to support the (health) department’s COVID response efforts,” county spokeswoman Rebecca Carter said.
Harris, the county’s health director, told elected officials in late June she needed more staff, saying a six-day work week for employees was not “sustainable” amid the pandemic’s duration. The county is now recruiting 30 more case investigators and prioritizing applicants who can speak another language, Carter said.
“The case investigation is definitely where we are seeing the most strain, just because we are having so many cases coming in,” Sullivan said. “Case investigation and contact tracing is a core part of our response, but it’s not going to be the only thing we focus on….We absolutely know that we are not capturing all the cases out there.”
Harris has said the actual tally could be 10 times as many lab-confirmed cases, due to asymptomatic spread of the virus. And Mecklenburg needs nearly 2,000 total contact tracers to manage the region’s large volume of cases, according to a George Washington University model. That is 12.5 times greater than the county’s current staffing levels
Since May, the sheer quantity of new cases has inundated the containment strategy, coinciding with the phased reopening of places like restaurants and churches where people have more opportunities to gather.
Certain health departments, like in Mecklenburg and Gaston counties, handle the bulk of the community’s pandemic response — in addition to more routine needs for lower-income residents, such as immunizations and family planning clinics.
But in Union and Cabarrus counties, for instance, some COVID-19 interventions are outsourced to the state. Still in other sparsely-populated parts of North Carolina, a health department or health alliance might manage coronavirus outbreaks for two or more counties.
“I feel like the extent we’re able do (contact tracing) really depends on how many positive cases we have,” Wright, of Gaston County, said. “We continue to cross-train people...At this point, there hasn’t been a problem.”
There have been nearly 140 confirmed cases for every 10,000 residents in Gaston County as of Tuesday, according to data from the state Department of Health and Human Services. In Mecklenburg, the rate is 195 cases per 10,000 residents, state data shows.
In Union County, the health department manages all case investigations, but relies on a state collaborative for contact tracing, said lead communicable disease nurse Ashley Burts. The county has recorded about 2,900 infections, according to state data.
“We did not have the capacity to do (contact tracing) in-house,” Burts said, adding the arrangement gives health department employees more flexibility to focus on outbreaks at congregate living settings.
Success stories
Catawba County announced its contact tracing triumph on July 9, releasing a detailed graphic that illustrated just how contagious coronavirus can be when health guidelines are ignored.
Catawba Public Health Director Jennifer McCracken said the crux of the investigation revolved around just one infected person and a mention of the family gathering. Shortly after, contact tracers realized spouses, coworkers, grandparents and an elderly neighbor were all impacted.
”We have learned the importance of what questions to ask,” McCracken said. “People feel bad about the situation, that they exposed their friends and family. We just want them to know it’s OK to talk to us.”
Contract tracing is better suited for those isolated events, where people can pinpoint their whereabouts and social interactions, many experts say. The approach also seems to apply well to COVID-19 outbreaks at long-term care facilities and childcare centers.
”Any place where it’s more contained, like a congregate living setting, where you generally have people who are there all the time, that’s probably the easiest place,” Burts said.
Clusters are common among households, too, with family members unable to completely isolate and avoid shared spaces with one another. In Gaston County, such clusters are a key focus area, Wright said.
Sullivan said in a Mecklenburg data analysis, about 11% of people who live with an infected individual have also subsequently tested positive for COVID-19. It is unclear if that higher infection rate disproportionately affects marginalized communities, such as Hispanic residents who often have larger households, she said.
But the more transient a situation becomes, such as people navigating a crowded bar or restaurant, the trickier it is for contact tracers to connect the dots of a possible COVID-19 cluster.
Patrons who momentarily brush by one another don’t necessarily qualify as close contacts, based on state guidelines. Restaurant employees, though, do fit the criteria.
Sullivan said Mecklenburg is closely monitoring and educating employers that routinely see coronavirus cases. Most employers in the Charlotte area, she said, are implementing the necessary safety precautions to keep their staff healthy.
Yet even in the county’s own Park and Recreation Department, officials didn’t know where some Mecklenburg County Aquatic Center employees became infected. In an email last month, County Manager Dena Diorio told elected leaders and top administrators that the four initial cases among lifeguards and supervisors were a “coincidence.”
The health department, Diorio said, determined how three of the workers “contracted the virus and it was not at work.”
A fourth case remained a mystery.
Less than a week later, a fifth case was reported and officials shut down the aquatic center.