Duke researchers discover how leukemia spreads to the brain
Patients combat leukemia, the most common childhood cancer,with chemotherapy — injections of anti-cancer drugs into the bloodstream.
But acute lymphoblastic leukemia, which makes up three out of four childhood leukemias and also affects adults, can infiltrate the defense wall between the bloodstream and the brain and hide in the brain or spinal cord and later reappear.
In a paper published last month in Nature, Duke researchers uncovered that acute lymphoblastic leukemia, or ALL, slips into a back door into the brain using specific molecules in bone marrow.
“One of my dreams is that we develop a molecular targeting to prevent ALL from migrating in,” said lead study author Dr. Dorothy Sipkins, professor at Duke. “Even when we do [preventative] chemotherapy, it doesn’t work for everyone; [some of] the people relapse after. It’s not enough for all the patients, so if there’s a way for us to do better, it’ll be a targeted treatment.”
How ALL cells slip into the brain
Think of your bloodstream as a subway that delivers nutrients and blood cells throughout your body. Only some molecules, like normal red blood cells, get through the high security of the blood brain barrier—most of the subway cars don’t open their doors at the brain stop. For over a decade, Sipkins searched for how ALL, which develops in the bone marrow, slips past security and enters the brain.
Unlike brain cancer or other cancers that metastasize, or move, to the inner parts of the brain, ALL is only found in the outer layers of the brain. This fact gives a hint of how ALL might enter from the outside of the brain rather than through the bloodstream.
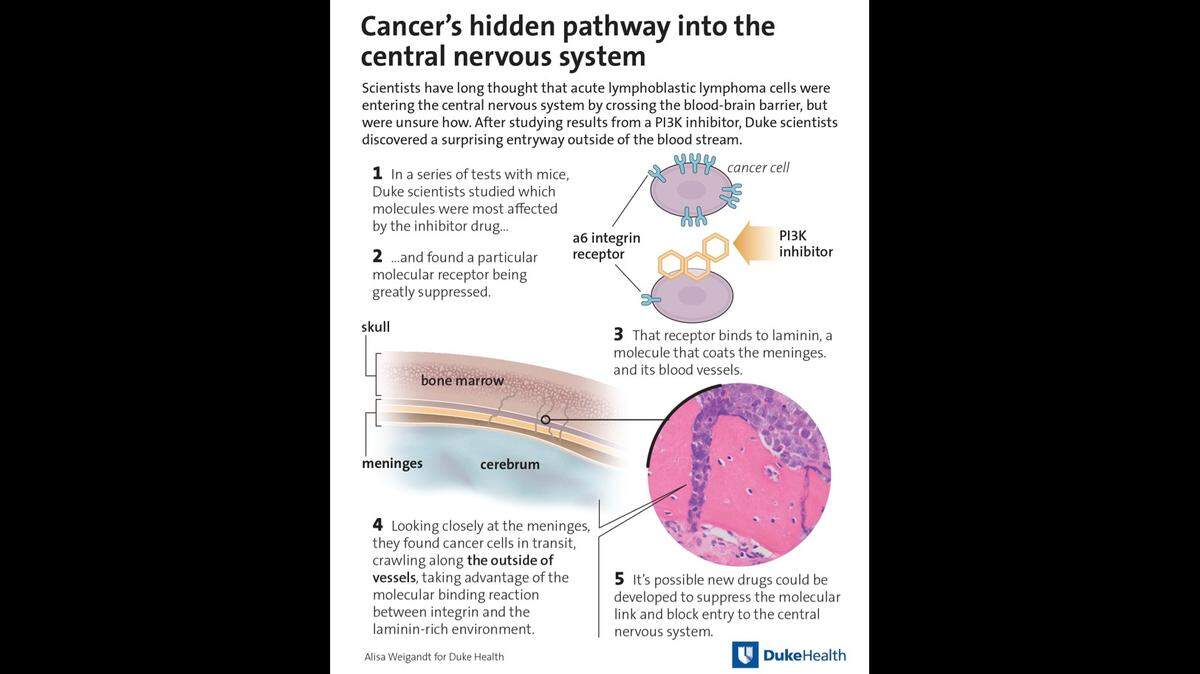
The culprit was a molecule called alpha six, which sits on the outside of ALL cells. Alpha six acts like magnetic boots, allowing ALL to cling to the outside of the subway car while it tunnels through bone marrow. The cells then slip straight into the station without going through the doors.
“The mystery was solved after years of trying to figure it out and looking in the wrong places, looking in the subway car, and we had to look outside the subway car,” Sipkins, who worked out the analogy with us, said. “It was like a big puzzle where we knew we were missing a piece and finally all the pieces fit together.”
The researchers happened upon the magnetic boots by accident. Sipkins’ lab was testing a drug on mice with leukemia. They realized that the mice never had a telltale central nervous system relapse. Relapse of the central nervous system, which is the brain and spinal cord, occurs in 5 percent to 10 percent of patients with ALL.
“We did a screen to see what molecules were being affected by this drug and that’s where alpha six popped up on the screen,” Sipkins said. “Alpha six is important for developing neurons that move about the brain. Those [leukemia] cells were using those boots the way that developing neurons would find their way in the developing brain.”
Sneaking past security at the blood brain barrier
In the blood brain barrier, blood vessels squeeze next to each other and stop other molecules from coming through. So chemotherapy drugs injected into the bloodstream don’t make it into the brain. Even if a patient has no leukemia cells in the rest of their body, ALL might still hide out in the brain, relapsing after weeks, months or years.
“[Leukemia cells] survive chemotherapy and other treatments by hiding out in the nervous system, and they’re undetected and untreated and they can survive to go to other places in the body,” said Dr. Matthew Foster, section chief of leukemia at the UNC Lineberger Comprehensive Cancer Center. “It’s a reservoir untouched by chemotherapy.”
Central nervous system relapse is a pernicious feature of ALL. To avoid it, doctors inject preventative chemotherapy drugs into patients’ spinal cords, bypassing the blood brain barrier.
“The reason we do it in the spinal fluid is because drugs don’t penetrate into the brain,” Sipkin said. “Sometimes it requires giving very high doses in the bloodstream to get past the blood brain barrier, but it’s a really unpleasant process to put it directly in the spinal fluid.”
High doses of chemotherapy cause a host of issues for patients, including kidney damage, mouth sores and other organ damage, Foster said. Without the invasive preventative dose, 30 percent to 70 percent of patients will get ALL in their central nervous systems, according to the paper.
“If you think about cancer in general, like breast cancer for example, in an extreme case you can do a surgery and just remove the cells,” said Dr. Jaíra Ferreira de Vasconcellos of the Henry M. Jackson Foundation for the Advancement of Military Medicine in Maryland. “In brain surgery you can also do that, but the consequences are much more dramatic. The brain is a part of our body, and the blood brain barrier is there to protect it.”
Future applications
The American Cancer Society estimates that North Carolina will see 2050 new cases of all kinds of leukemia this year and 760 deaths.
“The alpha six might be very specific to ALL, but other types of leukemia may use the same mechanism,” said de Vasconcellos. “[This study] could shed light on other cancers that infiltrate the nervous system.”
Adult patients whose ALL pops back up in the central nervous system survive on average six months after relapse. Finding out how ALL gets into the spinal cord and brain can help researchers save lives by preventing relapse.
In the paper, Sipkins’s lab experimented with a drug that blocks alpha six, “demagnetizing” the boots and stopping the leukemia cells from entering the central nervous system. Further research and development might show how to turn this molecular targeting into a viable treatment strategy, she said.
“Many of the pediatric ALL is highly curable; the vast majority of children are cured of this leukemia,” said Foster, the doctor at UNC. “However, one unsolved pattern of failure has been recurrence in the central nervous system. This paper may be a first step in tackling one of the last unsolved problems in childhood acute lymphoblastic leukemia.”
This story was originally published August 8, 2018 at 6:44 PM with the headline "Duke researchers discover how leukemia spreads to the brain."