Local COVID-19 tests hit plateau. Meck seeks asymptomatic people for more testing.
Mecklenburg County must expand coronavirus testing to better mitigate outbreaks and to detect how many asymptomatic residents could be unknowingly infecting others, Public Health Director Gibbie Harris says.
Up to 40% of people with COVID-19 may be asymptomatic, Harris said this week. Recent CDC guidance affirms that estimate.
“We really need more testing of individuals that are not just feeling ill or know that they’ve been exposed but are in environments where they may have been exposed,” Harris said during a news conference Wednesday.
Another dramatic ramp-up to local testing, though, faces hurdles.
Hospitals, clinics and drive-thru testing services are administering an average of more than 25,000 COVID-19 tests per week locally, according to the most recent public health data available. A Charlotte Observer analysis of the data shows the average number of COVID-19 tests per day in June doubled, compared to May.
Capacity increased again last month — but not by as much.
Now, volume appears to have plateaued — and been stuck — at around 3,500 to 3,800 tests per day.
“The more we test, the more we know about what’s going on in our community,” Harris said during a news conference Wednesday.
“What we’re focused on is making sure we’re making (testing) as readily available as we can in our community...as well as increasing (testing) sites, especially in places where we know the positivity rate is higher.”
In April, Atrium Health and Novant Health launched mobile testing sites throughout Charlotte to reach communities who have been disproportionately impacted by the coronavirus.
Hispanic residents account for almost one-third of the caseload, despite making up just 14% of the county’s population, based on 2019 U.S. census estimates. Mecklenburg officials say the high rate is partially due to “targeted testing occurring in neighborhoods with lower access to care,” in addition to more Hispanic residents living in larger households and working at essential jobs.
Coronavirus testing is a crucial tool to gain control of the pandemic, particularly before cases spiral uncontrollably, officials say. More aggressive testing allows health departments to wield other time-sensitive intervention tactics — like contact tracing to break the chain of viral transmission.
In the Charlotte area, according to Harris, testing is readily available and turnaround time for results has shrunk from nearly one week to 72 hours or less. At certain sites, testing is typically free for people without insurance.
Still, she dissuades businesses from requiring that returning employees pass a COVID-19 test, which could lead to a person seeking a test multiple times, straining resources.
Unlike earlier in the pandemic, testing is not limited to people with the worst of symptoms or who have traveled to an international hotspot.
Testing criteria in North Carolina is broad and includes:
▪ People experiencing COVID-19 symptoms or who had close contact with an infected individual
▪ People with a high exposure risk to the virus, based on their job or living environments, as well as underlying illnesses
▪ People who attend a large gathering, including protests
Testing people with a range of symptoms and possible exposure risks is critical, Harris said, as health officials grapple to understand the extent of the ongoing pandemic.
Stagnant testing capacity may muddle key coronavirus metrics — including the daily tally of lab-confirmed cases and the percentage of tests that return positive COVID-19 results — officials rely on to guide reopening decisions.
Locally, with each gradual stage of reopening, health data shows that a worsening positivity rate and caseload are closely linked with less social distancing.
But wider access and capacity for testing can help drive down the region’s positivity rate and simultaneously empower health officials to warn people with no symptoms they may be contagious.
Still, a nationwide shortage of testing supplies has directly hindered Atrium’s efforts, CEO Gene Woods testified last month to the U.S. Senate Special Committee on Aging. The hospital system is equipped to conduct 4,000 tests daily, but can manage only 20% of that load with the available reagents.
“We realize the road ahead is long and there’s many challenges that remain,” Woods testified. “Opportunities remain to significantly expand testing supplies, so that we can care for more people, especially the elderly, and we stand ready to be part of that solution.”
Dr. Sid Fletcher, Novant’s chief clinical officer, reiterated that some developments surrounding testing are encouraging.
“I think we’re hitting a pretty good mark of being able to test everyone who needs a test (and) who’s asking for a testing,” Fletcher told the Observer recently.
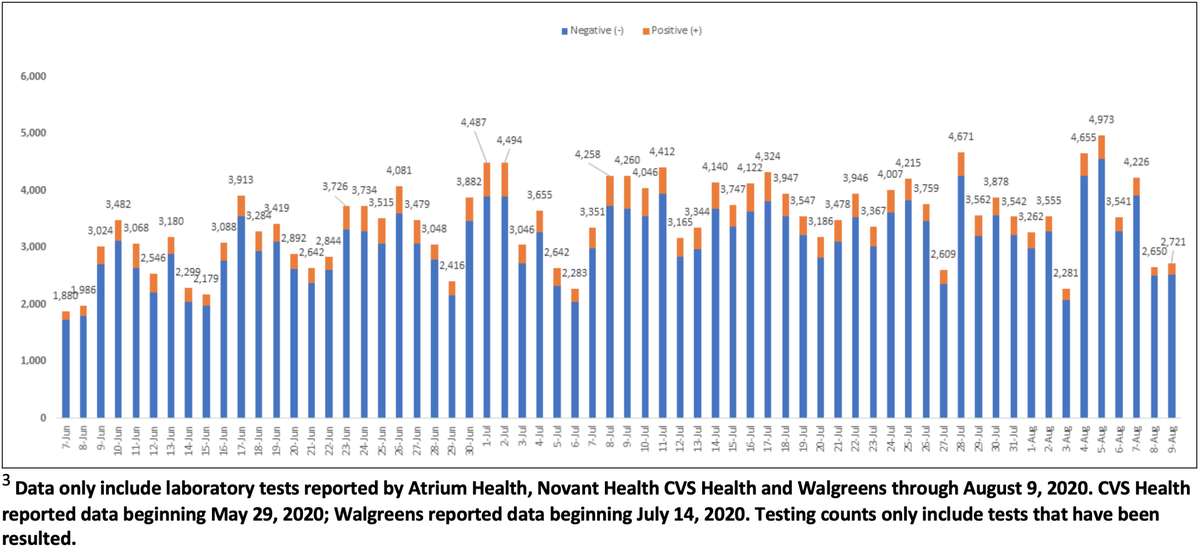
A slower ramp-up
Testing capacity has dramatically increased since mid-March, when Mecklenburg County was receiving just three test kits at a time from the state.
In April, about 660 people were tested each day in Mecklenburg. That volume more than doubled in May to about 1,500 daily, and again in June to almost 3,000 daily.
In July, the daily testing average climbed to only about 3,700.
Mecklenburg health officials release new data on the amount of testing twice a week. The reach of testing ebbs and flows day to day.
Last Wednesday, for instance, officials say 4,973 tests were administered — a record high for the county. Two days prior, just 2,281 people were tested, one of the lowest-volume days in the past two months.
Since late spring, state health authorities have told Mecklenburg that a higher proportion of all county residents must be tested for COVID-19.
For example, in early July, the state established a 12.5% testing goal for Mecklenburg and eight other North Carolina counties. Locally, that goal meant the county needed to test about 140,000 people over a 30-day period.
NCDHHS says the minimum testing threshold for all local health departments is 5%, according to department spokeswoman Kelly Haight. But Mecklenburg and eight other counties had much higher testing targets due to “concerning trends in viral activity,” Haight told the Observer Thursday.
Gov. Roy Cooper on Thursday said more testing — as well as subsequent contact tracing and isolation orders — are key to slowing the spread of COVID-19.
Not enough testing, in turn, means greater obstacles for North Carolina to flatten the coronavirus curve.
Epidemiologists say a high test positivity rate signals that there’s not adequate testing in a region. Mecklenburg’s rate — which averaged 11.4% in early July — has slowly declined to 7.5% in the last week, according to county data. But it is still above the 5% infection rate the state wants to see before allowing more businesses to reopen and getting all children back to school.
Harris has declined to specify a target for Mecklenburg, despite county commissioners calling for a concrete number as they also grapple with imposing more coronavirus restrictions on residents. Harris said Wednesday she’s not holding her breath to hit a 1-2% positivity rate — a figure currently seen in parts of the Northeast.
This story was originally published August 14, 2020 at 10:14 AM.