Urgency and scarcity: The coronavirus has NC nurses and doctors working hard, but wary
READ MORE
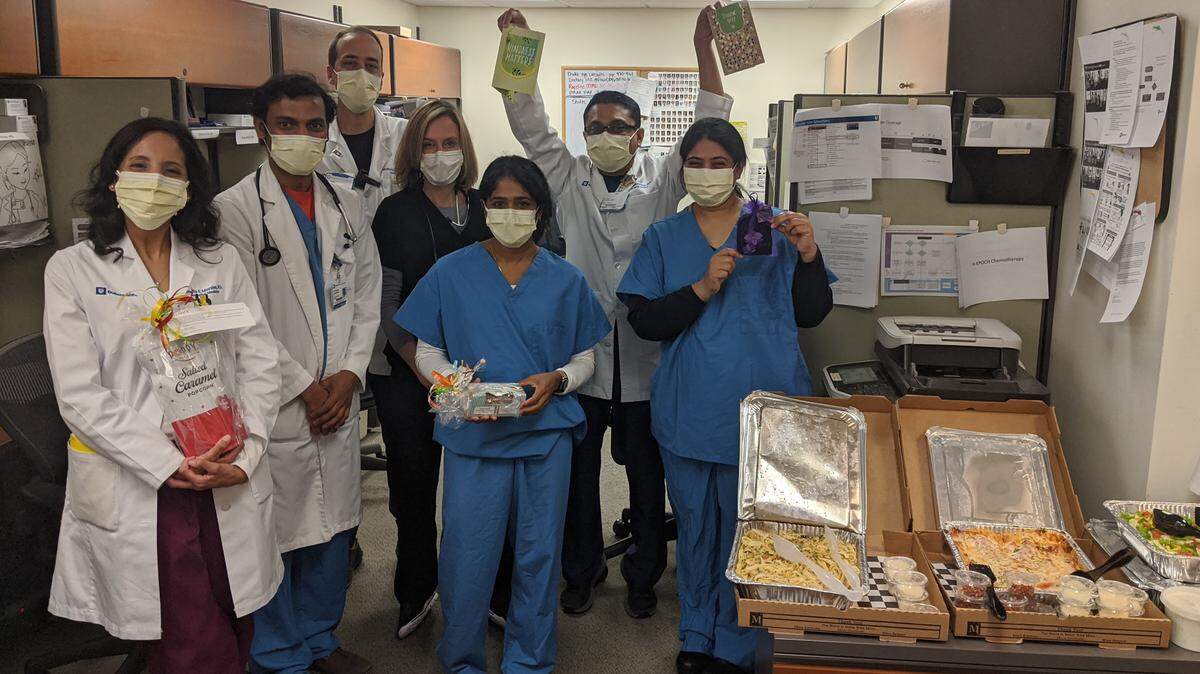
Healthcare Heroes
The News & Observer is telling the stories of “Healthcare Heroes,” those on the frontlines of treating coronavirus patients. Others are managing the equipment that allows those patients to be treated safely. These workers are putting their own health and the health of their families at risk every day so they can help others. Here are their stories.
Expand All
They have a camaraderie borne from doing an essential job, but with a layer of anxiety knowing that that work presents a potentially fatal threat. They are developing new procedures to protect and treat patients efficiently, with a wary eye on the low supply of protective gear.
Hospital staff are at the front lines battling the easily spread and sometimes deadly coronavirus, and they say they know, looking at projections, that this is just the start. Hospitals and their staffs have changed the way they work to prevent the pathogen’s spread to patients not infected with the virus and to keep it out of their own homes.
Some hospital innovations were driven, in part, by the need to preserve protective equipment.
UNC Healthcare looked at ways to test people for the coronavirus so they wouldn’t have to go into a clinic and come into contact with patients who aren’t infected.
The original idea was to do the testing in trailers, said Dr. David Wohl, a professor of medicine at UNC-Chapel Hill and an infectious disease specialist. But that idea was scrapped because of the low supply of masks.

Staff pivoted quickly to set up a drive-thru, he said.
“Within a day, they devised a whole new plan,” said Wohl, who is working at the drive-thru testing site in Chapel Hill. Testing people through car windows means that practitioners don’t have to shed all their protective gear after each patient, he said. They just have to change gloves.
Wohl described the experience as “flying a plane that’s being built as we fly it.”
“Nobody complained,” he said. “Everyone’s been flexible.”
“The hard part for us is everything we’re doing is really dealing with a circumstance where there is scarcity. That has pretty much been part of everything we do,” he said. “UNC has done a really good job of standing up what we could given what we have.”
Apart from family
He puts in long hours these days: “I haven’t worked this hard since I was an intern,”said Wohl, 56. And it comes with the worry about carrying the virus home to his family. Wohl said he is lucky to have an apartment attached to his house, where he stays during some of his down time. When he sees his family, he keeps his distance.
“When I’m inside, I am more than six feet away from everybody,” he said. “There’re no kisses. There’s no touching. I’m really conscientious about washing my hands frequently. I’m checking my temperature twice a day. So many of us do. That’s just the new normal for us now.”
Cortney Hart, a nurse living in Willow Spring, has no choice but to bring a family member with her to work at the UNC Rex emergency department. Hart, 36, is 16 weeks pregnant with her third child. She posted a lighthearted photo of herself and three pregnant co-workers, all wearing masks, with hashtags #myppeisnotjustforme and #wecantstayhomebutyoushould.
Hart said the hospital gave her the option of moving to another assignment, but she feels well-protected and wanted to keep working in the Emergency Department.
“I wouldn’t be anywhere else,” she said. Hart said she’s being kept away from the sickest patients, and those suspected of having COVID-19 are placed in a blocked-off area.
Hart said getting supportive comments on her Facebook post “feels absolutely great.”
“People are calling us heroes. I don’t know that we’re all that. We’re just doing what we do everyday. It’s just that more of it shows.”
Bending the curve?
Nurses and doctors have taken to imploring people to follow directives to stay at home or, when they venture out, to stay far from other people to slow the spread of the coronavirus, or “bend the curve.” The aim is to prevent a spike in cases that will overwhelm hospitals.
Numbers over the last week look like the social distancing tactics may be working in North Carolina, Dr. Doug Trocinski said. But, he said, it’s way too soon to celebrate.
“I applaud people,” said Trocinski, chief medical officer at WakeMed Cary and an emergency room doctor. “North Carolina got out in front of this very early. It’s incredibly inconvenient and difficult — the social distancing and the businesses taking a furlough — but it looks like it actually may be working. It can make a huge difference. It won’t change the number of people (who get sick) but we’re not going to get it at the same time. If that’s the case, we can manage that.”
Dr. Meera Udayakumar, medical director of the hospitalist program at UNC Rex, said it’s too soon to tell whether the curve is bending. “We need to keep doing what we’re doing with the social distancing efforts and more to give us time to prepare,” she said.
Researchers at the University of Washington forecast a peak in North Carolina cases at the end of this month. The state is behind other locations — New York City, for example — that have seen a surge. That’s given North Carolina hospitals time to prepare.
“We have the opportunity to learn from their experience,” Udayakumar said.
The News & Observer wants to share your stories about COVID-19 and the North Carolina health care system. Are you a doctor, nurse or patient? Share your story or contact us here.
Supply of ventilators
There’s been a national focus on the supply of ventilators, machines that hospitalized and critically ill COVID-19 patients need to help them breathe.
Dr. Francis Castiller, who leads the critical care team at UNC Rex, said the hospital has few COVID-19 patients now, but is preparing for the surge.
“We have the same concerns and struggles I think the entire world has,” Castiller said. “Looking at current inventory, our capacity is quite high. When a surge comes, the demand is going to outpace the supply.”
The hospital is working hard to get more ventilators, Castiller said, and may use other breathing machines, such as ventilators used in operating rooms that can be repurposed.
Trocinski said he’s a part of a task force at WakeMed whose members are scouring the globe and working with other health-care systems to find protective equipment they’ll need in the coming weeks and months.
“Our people are making orders and making contacts with people all over the world to try to mitigate the gaps we see down the road,” he said.
In the ICU
Sarah Eagle, an ICU nurse at the WakeMed Raleigh campus, is working her first nursing job out of school. She said her nickname is “Baby Nurse.”
Eagle, 22, said she feels properly protected in the unit. In addition to the gowns and gloves, staff members wear helmets that blow air to keep particles away from their faces.
Everyone is dealing with a learning curve, she said, because there’s new guidance constantly streaming from the Centers for Disease Control and Prevention.
Eagle said she feels some anxiety, but it’s not from her job.
“We’re just like the rest of the community,” she said. “We’re scared for the rest of our families, going to the grocery store. It’s not from the job. I don’t have any lack of protection.”
Hospitals have tried as much as they can to separate people who might have COVID-19 from other patients. For example, The News & Observer reported UNC Rex Hospital constructed a separate ICU for patients with respiratory disease.
Anastacia Jennings eagerly accepted a new job at UNC Rex Hospital as the acting clinical manager of the new special ICU. One of the reasons she could respond so quickly is that she was ready to devote hours to preparing for and managing the new unit.
“I personally don’t have animals or a husband or kids,” she said. “I really love leading people. I jumped at the opportunity because I thought I could help.”
Jennings said she’s working about 60 hours a week, but emphasized that that’s because she wants to. “The past 2 1/2 weeks have been completely energizing and at the same time, exhausting,” she said.
Preserving equipment
Planning for patient interactions is detailed, with special attention given to preserving protective equipment. That’s meant making sure what’s needed for patients is already in the room so staff members don’t need to go in and out to find things, which would require they change gowns every time, she said.
They also keep more supplies on carts near rooms, so that medical staff in a patient’s room can wave down a coworker and just reach a hand out the door for what they need.
Nurses are cleaning and decontaminating the unit, so housekeeping staff doesn’t need to come in. A big UV light is used to disinfect empty rooms.
Jennings said she thinks back to December, when she never thought twice about how many gowns or masks she was using.
The unit has the equipment it needs, she said, but people notice that supplies are not as well stocked as they were.
“Once you’re told you might not have enough of something, you really think about how to maximize the resources you do have,” she said.
There’s a sense on the unit of everyone ”pulling together to do amazing things,” Jennings said. That’s mixed with anxiety and the fear of the unknown or what’s to come, she said. “Are we going to turn into another New York City or China? Is that what our future will be?”
Wohl, the UNC infectious disease specialist, said there’s a sense of camaraderie in Chapel Hill as well. But there’s also a general sense of apprehension.
“I think everyone feels it,” he said. “There are so many unknowns. If you do get infected, will you have a mild case or a more severe case?”
He said he is “more and more frustrated” by the scarcity of protective equipment and knows other providers are, too.
“I do feel there is a monumental failure,” he said. “We have an agreement with our government to help us. At the highest levels, there has clearly not been a coordinated response to procure what we need.”
The nation squandered precious time in January, he said, when the coronavirus was spreading rapidly in China.
“It’s not just one piece of equipment we don’t have enough of,” he said. “It’s swabs, the masks we wear, all the things across the board have not been adequate. That’s just disturbing at many levels. There were delays in getting testing up and running. That really put us behind the 8-ball.”
This story was originally published April 2, 2020 at 9:29 AM with the headline "Urgency and scarcity: The coronavirus has NC nurses and doctors working hard, but wary."









.jpeg)