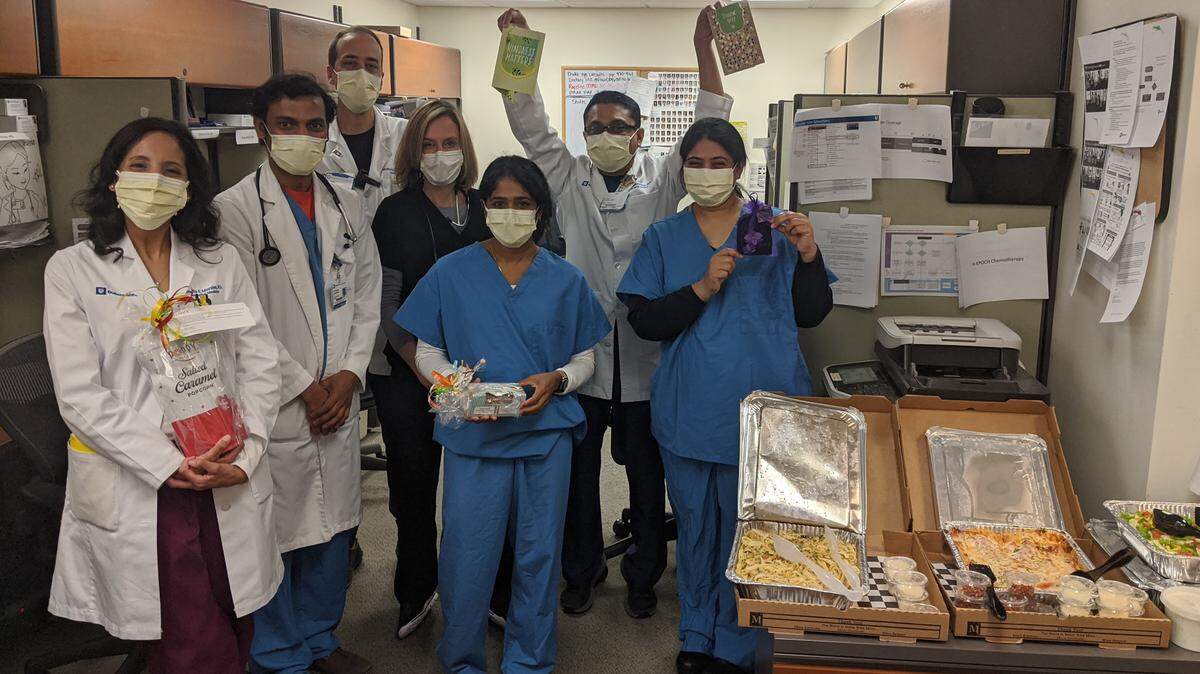
With visitors banned, hospitals devise ways to communicate with patients and families
READ MORE
Healthcare Heroes
The News & Observer is telling the stories of “Healthcare Heroes,” those on the frontlines of treating coronavirus patients. Others are managing the equipment that allows those patients to be treated safely. These workers are putting their own health and the health of their families at risk every day so they can help others. Here are their stories.
Expand All
Kensley Prouty was all of two hours old when her father, Michael, held her up to the window of the second-floor room where his wife, Jill, was resting in the birth center at UNC Rex Healthcare.
Outside, below, were Michael’s parents, standing near the hospital loading dock waving and crying and trying to catch a glimpse of their new granddaughter. The family calls this their “Lion King” moment, the way newborn cub Simba was held up on Pride Rock before the other animals.
“All we needed was the red mark across the forehead,” Jill said.
Families, doctors and others at hospitals are devising new ways to communicate during the coronavirus pandemic. Hospitals have all but banned visitors, even for non-COVID-19 patients, to prevent the virus from spreading. That has eliminated close, face-to-face encounters at a time and in a place where people want them most.
Jill Martin-Prouty wanted her in-laws in the room, to hold their granddaughter and perhaps rock her to sleep while Jill took a nap. But the wave from the driveway outside was the best they could do.
“It was like, ‘Hey we’re here for you even though we can’t be in there with you,’” Jill said.
The substitute for in-person communication is usually digital — a video chat over a cellphone or a computer. Most patients have the devices they need, but for those who don’t, hospitals are now providing tablet computers so patients can both see and hear loved ones who can’t visit.
Duke University Health System has about 1,500 iPads available for patients, including 1,000 it purchased since the coronavirus outbreak began, said Matthew Roman, chief digital strategy officer. A couple hundred of them have been put to use so far, Roman said.
“It’s not the human touch,” he said, “but it’s as close as we can do right now.”
The devices also allow doctors and other health care workers to communicate with patients without entering their rooms, which saves on precious masks, gowns and other personal protective equipment.
“If I have to walk into an isolation room to simply ask a question, I have to gown up completely,” Roman said. “But if can ring the room and have a face-to-face video connection, then I can save that PPE.”
At other times, as teams of physicians, nurses and therapists make their rounds from patient to patient, only one has to go into the room in full PPE, while the rest communicate from outside on video.
With nurses, doctors and others all wearing masks and shields, video conferencing can actually be more personal, said Paula Carter-Scott, a registered nurse who is helping WakeMed improve communication during the outbreak. WakeMed is using Google Hangouts and Cisco’s Jabber software to speak with patients in isolation.
“Video chatting lets the patient see their nurse as a smiling person instead of a figure who is all garbed up,” Carter-Scott said. “If the patient just has a quick question, answering it with Jabber also saves PPE and the time spent donning and doffing it.”
UNC Rex recently launched a tool that’s embedded in patient electronic records that allows doctors to chat with them by video. Dr. Seth Weinrab, a general surgeon and the hospital’s chief medical information officer, said Rex is trying to make the medical rounds-by-video feel like they do when doctors meet at a patient’s bed.
“We’re working hard to make a virtual experience add up to a bunch of people in the room,” Weinrab said.
Chaplains minister by video
The bans on hospital visitors are especially hard when patients are in for long stays or in the final days of their lives. Noel Hammond, a registered nurse at WakeMed, used Google Hangout to allow a family to visit virtually with a man during the last days of his life in the hospital.
“I understood that they just wanted to see his face and tell him that they loved him during the end of his journey,” Hammond said.
Rev. John Oliver, director of chaplain services at Duke University Hospital, said the coronavirus outbreak hasn’t changed the goal of a chaplain’s work, to listen to patients and their families and to support their spiritual journey as they wish.
But now Oliver is usually doing that by phone or computer. He uses the computer to share a prayer or show family what the room looks like and what the patient can see out the window.
“Sometimes my job is simply holding the iPad and letting the family connect,” he said.
Oliver said chaplains and hospital staff find other ways to make these connections. The wife of a terminally ill man asked if they could play a favorite Christian song for him, because she had been listening to it over and over again and thinking of him. When families ask if they can send flowers or chocolates, Oliver has to say no but then encourages them to email photos that he can print and take into the room.
“That’s not super high tech, but it is a way to help family members feel like they’re connecting with their loved one,” he said. “They’re telling stories through these pictures.”
Doctors must communicate from afar, too
The physical distance is hard on doctors and other health care workers, too. Bedside huddles with patients and family members are all but gone; no one is in the waiting room eager for an update. Talking to patients by phone or by video is not the way many of them want to practice medicine.
“I like to be at the bedside,” said Dr. Abhi Mehrotra, who helps oversee emergency departments at UNC Health hospitals in Chapel Hill and Hillsborough.
But Mehrotra understands the need to preserve PPE and limits personal visits. He tells patients to keep their phones on and expect a call or in some cases communicates over baby monitors in the rooms, like “a simple walkie-talkie.”
“It’s not the ideal scenario and not how I choose to practice on a regular basis,” he said. “We’re trying to strike that balance.”
The amount of digital communication with family members varies from patient to patient, said Dr. Meera Udayakumar, who leads the UNC Rex hospitalist team, which manages a patient’s care during a stay at the hospital. Some want their families involved at each step and will call when a doctor is in the room. At a patient’s request, nurses, doctors and physician assistants will schedule time each day to call family members for updates.
“It’s been a big shift,” Udayakumar said. “We’ve always been a very patient- and family-centered hospital accustomed to having those conversations face-to-face.”
Oliver, the Duke chaplain, said patients and their families say they appreciate the efforts to stay in touch.
“Everybody understands why; there’s just no playing with this, and they get it,” he said. “Are they happy about it? No.”
Still, Oliver thinks iPads won’t disappear from patient rooms after the coronavirus pandemic is over. There are always family members who can’t visit in person, because of distance or other circumstances, and video conferencing will be a ready option.
Roman, Duke’s digital strategy officer, expects iPads will become standard issue in hospital rooms. Duke has developed a system to clear, clean and disinfect the computers just as they would the sheets and pillows.
“It’s like a new device,” he said. “It becomes part of normal workflow and a part of normal admission and discharge from the hospital.”
This story was originally published April 23, 2020 at 5:35 AM with the headline "With visitors banned, hospitals devise ways to communicate with patients and families."










.jpeg)